Arthritis in Midlife: What Helps and What Makes It Worse
Jan 21, 2026
About four months ago in Karate practice, I was trying to execute a 360 roundhouse kick (it's as insane as it sounds). My knees went one way; my feet didn't take the cue and follow along. A few hours later, I found myself in the ER with two torn meniscus. "Take it easy," advised the doctor. "Oh, and by the way -- you have arthritis in both your knees."
He said it as if that statement was going to take me down.
Fast forward to today: my tears are recovered, my black belt hangs in my closet, and I lift heavy weights in spite of my arthritis diagnosis. I'm not being flippant about arthritic pain, since I've had it in my hands and back, and was diagnosed seven years ago with early onset arthritis. But here's what I know now about arthritis that might change how you approach joint pain and aches as you age.
"Be Careful. Slow Down."
If you’ve been told you have arthritis, chances are you were also told—directly or indirectly—to be careful, slow down, or even avoid weight-bearing exercise.
But, hello — the science is in. We now know that advice is outdated.
Here's the truth: movement—especially the right kind of strength and weight-bearing exercise—is one of the most effective ways to reduce arthritis pain and protect your joints long-term. Read that again. Our tendency is to protect ourselves, stay comfortable and not do weight-bearing exercises in the face of arthritic pain, when that very inaction promotes more pain.
Let’s break down what the science actually says, what helps, what to be cautious with, and how to move confidently if you’re living with arthritis.
First, what type of arthritis are we talking about?
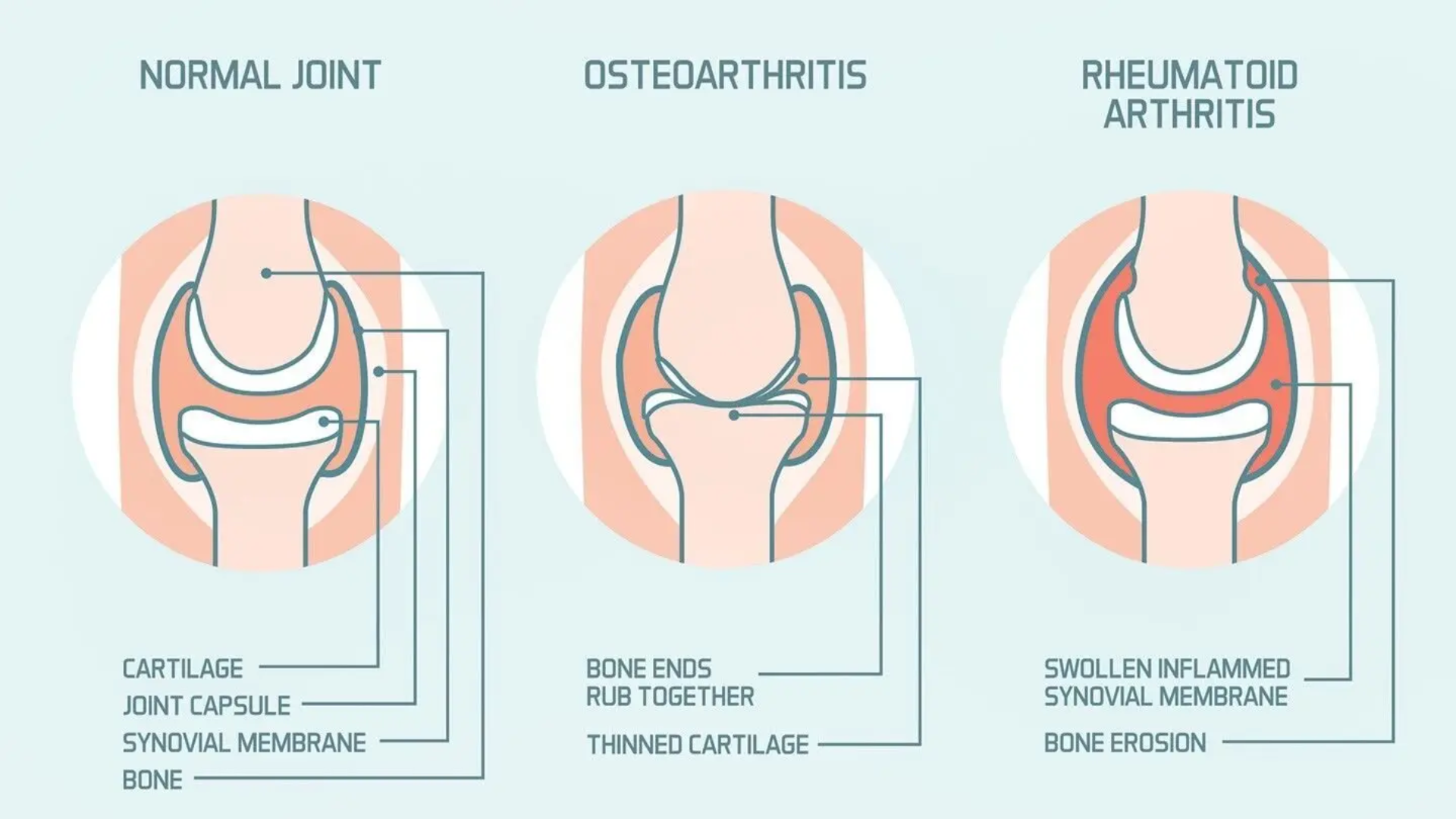
Arthritis isn’t one condition—it’s an umbrella term. The most common types include:
-
Osteoarthritis (OA): Often called “wear-and-repair,” and the most common form in midlife
-
Rheumatoid arthritis (RA): Autoimmune and inflammatory
-
Other inflammatory forms: Such as psoriatic arthritis
The recommendations below apply to most people with osteoarthritis and to those with well-managed inflammatory arthritis (always coordinating with a healthcare provider during active flares).
The outdated advice (and why it doesn’t work)
As I said, for decades, people with arthritis were told to rest their joints and avoid loading them. I remember my mom's best friend, Camilla, had terrible arthritis. Her hands were badly deformed from the condition, and she would often cry out in pain when she would have to open a jar or do something that required mobile dexterity and strength. It was heartbreaking.
We now know that this approach often makes things worse. Too little movement leads to weaker muscles, which means less joint support, increased stiffness, more pain over time, and just like Camilla experienced, faster loss of mobility and independence.
The truth is, our joints thrive on movement. When our muscles weaken, joints absorb more stress—and our pain increases.
Can you do weight-bearing exercise with arthritis?
Yes—and in most cases, you should.
Weight-bearing and resistance training are now considered cornerstones of arthritis management. What!? It's true. Strength training actually helps with arthritis and pain. If the logic above made sense, this correlary argument will also make sense: strong muscles help to reduce stress on your joints, and movement improves joint lubrication (synovial fluid). The more stability you have, the lower your pain and injury risk levels. Strength supports bone density and regular loading decreases pain sensitivity over time.
A simple rule to remember: strong muscles protect joints.

The best types of exercise for arthritis
What can you do for arthritis? Start with strength & resistance training. This doesn’t necessarily mean lifting heavy or training like an athlete (though I find no fault in that). You can start with exercises like air squats into a chair or bench, and step-ups. Work on executing light to moderate deadlifts (with good form), ensuring that you're increasing your repetitions (or "reps," in gym-bro speak) and progressively adding heavier weight once you feel comfortable at your level. It means hitting the resistance machines and working with dumbbells, kettlebells or resistance bands. You can even do slow, controlled bodyweight exercises (like plank, pushups, wall-sits, and more).
Consistency matters more than intensity. Progressive loading—done gradually—is key.
Next, increase your low-impact weight-bearing movement. This is especially great for daily movement or flare-sensitive days. Throw on a weighted vest and walk or hike. Do the elliptical or the stair climber at the gym, or try water walking as an alternative. These all support joint health, bone density, and circulation, and they help to 'floss' your joints with movement and mobility, which will help with the stiffness and pain.
Third, mobility exercises! Gentle joint circles where you take your joints through their full range of motion (with no pain), yoga poses (downward dog, pidgeon pose and cat-cow are brilliant), and a daily stretching routine are perfect, here. Try my morning flexibility routine, which helps to encourage blood flow and circulation. A helpful mantra: motion is lotion for joints.

What to be cautious with:
Certain activities may increase irritation if introduced too soon or done excessively. You'll want to be cautious with high-impact running on hard surfaces, jumping and plyometrics, high-rep, repetitive joint loading, and/or poorly coached HIIT workouts
You shouldn't ignore these, because they're incredibly beneficial to musculo-skeletal health, and you should plan to incorporate these into your movement regimen as part of aging well, but just be aware that these aren't usually the starting point for managing arthritis pain. So, don't avoid these; just don't start with these.
How to gauge pain safely: the 24-hour rule
Pain doesn’t automatically mean damage—but it is feedback. Use this guideline if you have arthritic pain:
-
Mild discomfort during or after exercise: acceptable
-
Soreness that resolves within 24 hours: okay
-
Pain that worsens or lingers beyond 24 hours: scale back (not stop)
Remember, you don't earn bonus points if you push through the pain (I'm speaking to myself, here). Progress comes from listening and adjusting, not blindly continuing.

Other tools that genuinely help arthritis pain
Heat and cold
-
Heat: stiffness and chronic ache
-
Cold: swelling and acute flares
Nutrition
-
Low to no added sugars
-
Minimizing ultra-processed foods
-
Adequate protein to support muscle
-
Omega-3 fats for inflammation control
-
Stable blood sugar (avoid sugary foods and go for a 15-minute walk after meals)
Sleep
Poor sleep increases pain sensitivity and inflammation. Getting between 7 - 9 hours / night helps your body repair. Sleep is therapeutic.

The bottom line: Movement is Healing for Arthritis
When joints are supported by strong muscles, good mechanics, and consistent movement, pain often improves and function is preserved.
Avoiding movement may feel like the better and safer short-term solution, but it accelerates decline over time. Lean into weight-bearing movement, and fight to keep your strength and mobility. You'll be rewarded with long-term joint resilience—regardless the diagnosis.
This article is for educational purposes and does not replace personalized medical advice. Always work with a healthcare professional if you have inflammatory arthritis, recent injury, or worsening symptoms.
Did you like this article? Leave me a comment and let me know!
x
Juliana






